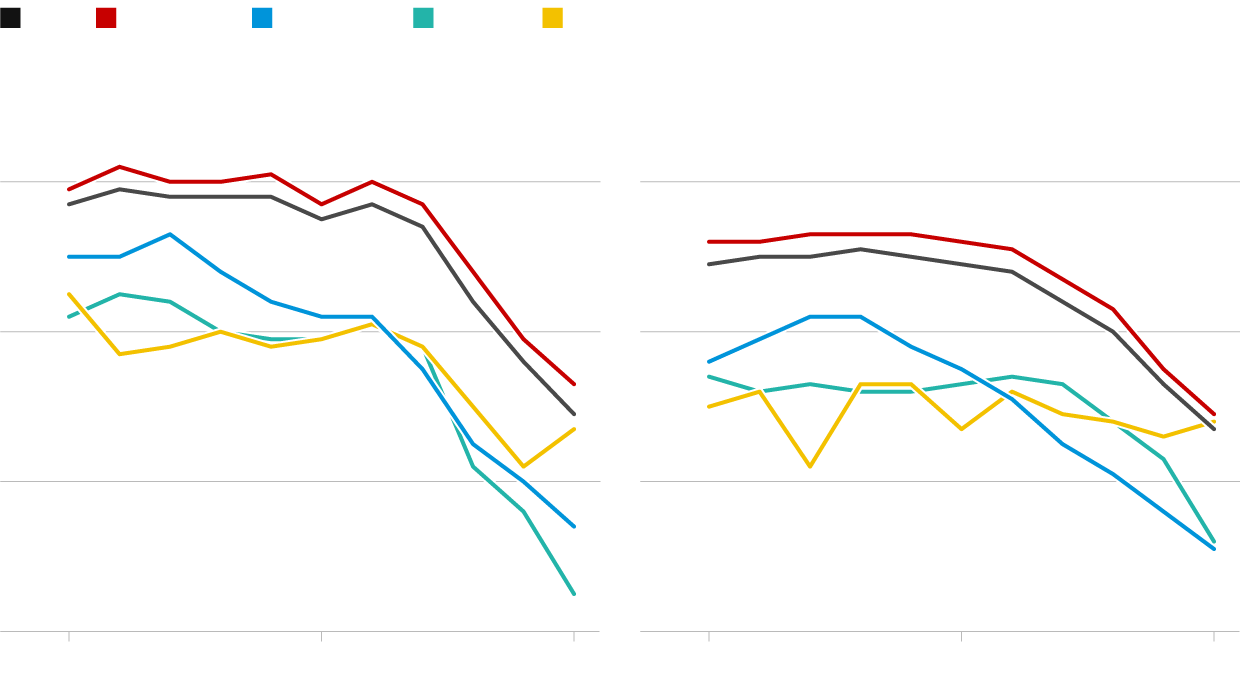
UK Healthy Life Expectancy Falls by Two Years in a Decade as Chronic Illness Crisis Deepens
People in the United Kingdom are spending fewer years in good health than at any point in the past decade, according to a new analysis that has laid bare the scale of the country's chronic illness crisis. Healthy life expectancy — the number of years a person can expect to live in good health — has fallen by approximately two years over the last ten years, dropping to just under 61 for both men and women. The UK is one of only a handful of wealthy nations to have experienced such a decline, and the fall has been among the steepest of any comparable country.Background
Healthy life expectancy is a more meaningful measure of population health than overall life expectancy, because it captures not just how long people live but how well they live. A society in which people live to 85 but spend their final 25 years in poor health is very different from one in which people live to 80 but remain healthy and active until the end. The distinction matters enormously for individuals, for families, and for public services — particularly the NHS and social care system, which bear the cost of managing chronic illness.
The UK's record on healthy life expectancy has been a source of concern for public health researchers for several years. While overall life expectancy has remained broadly stable — men can expect to live to around 79, women to around 83 — the proportion of those years spent in good health has been declining. The causes are multiple and interconnected: rising rates of obesity, the long-term effects of the Covid-19 pandemic, growing mental ill-health particularly among younger people, poor housing, and the persistent effects of poverty and deprivation.
The regional disparities in healthy life expectancy are particularly stark. The gap between the healthiest and least healthy areas of the UK has been widening for decades, reflecting deep-seated inequalities in income, housing, education, and access to healthcare. These inequalities are not inevitable — they are the product of policy choices — and their persistence represents one of the most significant failures of public health policy in the modern era.
Key Developments
The analysis shows that the average number of years people in the UK spend in good health has fallen by approximately two years over the last decade, dropping to just under 61 for both men and women. The UK is one of only a few wealthy nations to experience a decline in healthy life expectancy, and its fall has been one of the steepest among comparable countries.
The regional disparity is profound: there is a gap of around 20 healthy years between the richest and poorest areas of the UK. Healthy life expectancy in Richmond upon Thames is around 70 years, compared to just 51 in places like Blackpool and Hartlepool. This means that a child born in Blackpool today can expect to spend nearly two decades more of their life in poor health than a child born in Richmond — a difference that is not primarily explained by genetics or individual behaviour, but by the social and economic conditions in which people live.
The factors cited for the decline include poverty, poor housing, rising obesity rates, the long-term effects of the Covid pandemic — including long Covid, which affects an estimated 1.9 million people in the UK — and growing mental ill-health, particularly among young people. The economic implications are significant: more people unable to work due to ill health places greater pressure on the benefits system and reduces the productive capacity of the economy.
Why It Matters
The decline in healthy life expectancy is one of the most important public health stories of the decade, and it deserves far more attention than it typically receives. The UK's performance is particularly troubling when set against comparable countries: France, Germany, and the Scandinavian nations have all maintained or improved their healthy life expectancy over the same period. The difference is not primarily explained by healthcare spending — the UK spends a comparable proportion of GDP on health to many of these countries — but by the broader social determinants of health: income inequality, housing quality, food security, and the strength of the social safety net.
The 20-year gap between the healthiest and least healthy areas of the UK is a damning indictment of the country's approach to health inequality. This is the third consecutive decade in which that gap has widened rather than narrowed, despite repeated government commitments to "levelling up" and reducing health disparities. Unlike Wales, which has embedded health impact assessments into its planning and policy processes, England has no equivalent mechanism for ensuring that policy decisions are evaluated for their impact on health inequality.
Local Impact
In Northern Ireland, healthy life expectancy figures mirror the UK-wide pattern of stark regional inequality. Areas of North and West Belfast, as well as parts of Derry and Strabane, have some of the lowest healthy life expectancy figures in the UK, reflecting the legacy of the Troubles, persistent deprivation, and the long-term effects of deindustrialisation. The Belfast Health and Social Care Trust has been working to address these inequalities through community health programmes, but the scale of the challenge is enormous. In the Republic of Ireland, the HSE has similarly identified significant regional disparities in health outcomes, with rural communities and areas of urban deprivation facing the greatest challenges. The Irish government's Sláintecare reform programme aims to address some of these inequalities, but progress has been slow.
What's Next
The government's forthcoming Health Inequalities Strategy, expected before the summer recess, will set out its approach to addressing the regional disparities in healthy life expectancy. The NHS's 10-year plan, currently in development, is expected to include specific targets for reducing health inequalities. The Office for National Statistics will publish updated healthy life expectancy figures for all local authority areas in England later this year. Public health researchers are calling for a cross-government approach to the social determinants of health, including action on housing, poverty, and food security.
Sources: Diabetes.co.uk | NHS England