£1.8 Million Study to Test AI Tool That Could Transform Prostate Cancer Diagnosis on NHS
A groundbreaking £1.8 million clinical study has been launched to test a new tool that has the potential to revolutionise the diagnosis and treatment of prostate cancer within the NHS. The VANGUARD PATH study, funded by Prostate Cancer UK, will evaluate the effectiveness of the ArteraAI Prostate Biopsy Assay in providing more accurate and personalised risk assessments for men diagnosed with the disease, with trials running across NHS sites in Oxford, Bristol, and Glasgow.Background
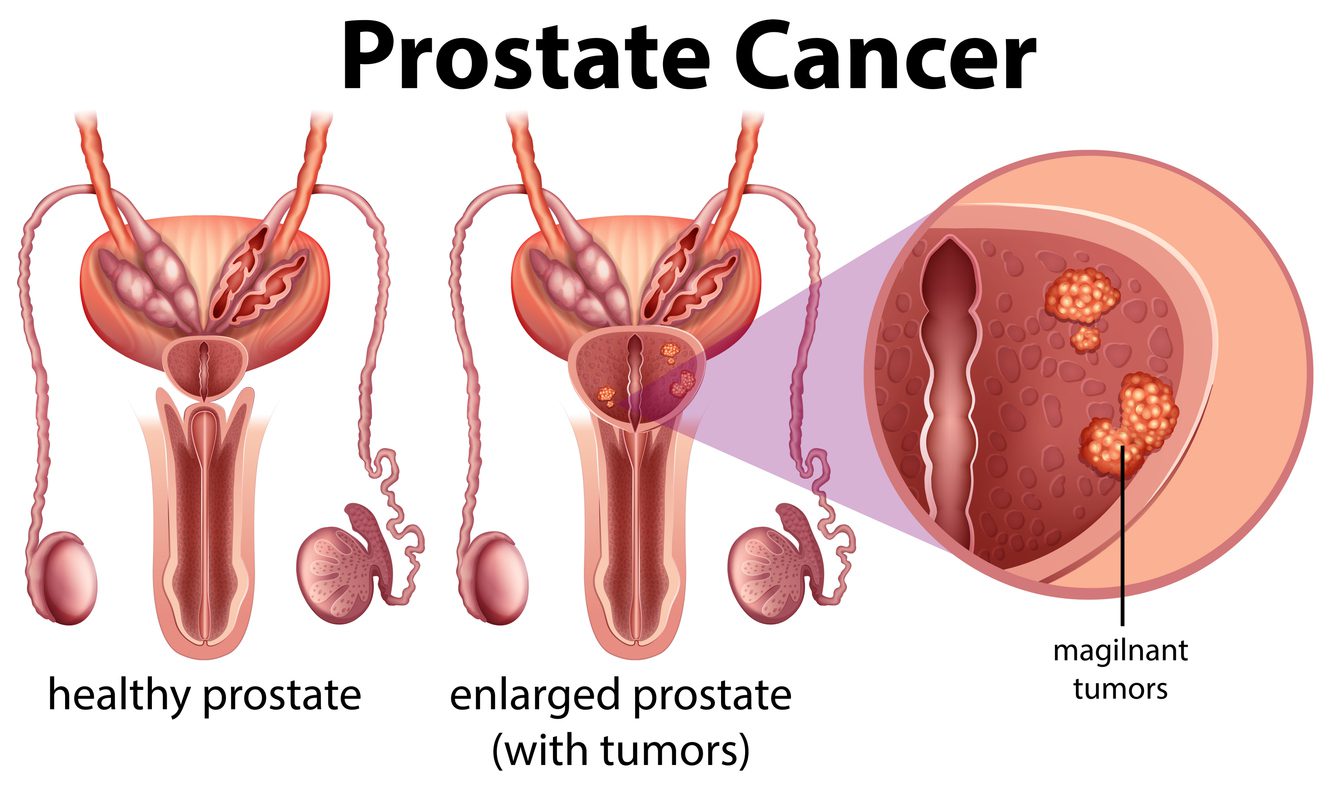
Prostate cancer is the most common cancer in men in the UK, with one in eight men being diagnosed in their lifetime. While survival rates have improved significantly in recent years, one of the biggest challenges in managing the disease is accurately determining the aggressiveness of the cancer at the point of diagnosis. The current system relies on a pathologist's visual examination of a biopsy sample and a scoring system known as the Gleason score, which can be subjective and lead to both over-treatment and under-treatment.
Over-treatment, where men with slow-growing, non-aggressive cancers are given intensive treatments like surgery or radiotherapy, can lead to unnecessary and life-altering side effects such as incontinence and erectile dysfunction. Conversely, under-treatment of aggressive cancers can have fatal consequences. There is a critical need for more precise diagnostic tools that can help clinicians and patients make better-informed decisions about the most appropriate course of action.
The VANGUARD PATH study, led by researchers at the University of Oxford and North Bristol NHS Trust, aims to address this challenge by harnessing the power of advanced digital pathology analysis. The study will focus on the ArteraAI Prostate Biopsy Assay, a sophisticated tool that analyses digital images of biopsy samples and identifies subtle cellular patterns that are invisible to the human eye. By correlating these patterns with long-term patient outcomes, the tool can generate a highly accurate prediction of how aggressive a particular cancer is likely to be.
Key Developments
The £1.87 million study will be rolled out across three major NHS sites in Oxford, Bristol, and Glasgow. The research will be conducted in several phases. Initially, the team will focus on implementing the tool and ensuring that it is compatible with existing NHS digital pathology systems and can produce consistent results across the different hospital sites. This is a crucial step in ensuring that the technology can be deployed at scale in a real-world clinical setting.
The core of the study will be a validation phase, where the tool will be used to analyse a large bank of historical biopsy samples from men who have at least five years of follow-up data. The researchers will compare the tool's predictions of cancer aggressiveness with the actual clinical outcomes of these patients. This will provide robust evidence of the tool's accuracy and its ability to outperform the current diagnostic methods. The study will pay particular attention to cases where there is currently high uncertainty, as these are the patients who could benefit most from the additional clarity provided by the new technology.
The final phase of the study will involve integrating the tool into the clinical workflow and gathering feedback from both clinicians and patients. The researchers will assess how the information provided influences treatment decisions and whether it leads to better-quality conversations between doctors and patients. They will also develop training materials to support the wider rollout of the technology across the NHS if the study is successful.
Why It Matters
The VANGUARD PATH study represents a significant step forward in the quest for personalised medicine. If the ArteraAI tool proves to be as effective as hoped, it could lead to a paradigm shift in how prostate cancer is managed. By providing a more objective and accurate assessment of cancer risk, the technology has the potential to spare thousands of men from unnecessary treatment and its associated side effects, while ensuring that those with aggressive disease receive timely and life-saving interventions. This would not only improve the quality of life for patients but also lead to significant cost savings for the NHS by reducing the burden of unnecessary treatments.
More broadly, the study is a powerful example of how advanced digital pathology is poised to transform healthcare. The ability of these tools to analyse vast amounts of complex data and identify patterns that are beyond human perception has the potential to improve diagnosis, treatment, and drug discovery across a wide range of diseases. The successful implementation of this technology in a major national health system like the NHS would send a strong signal about the readiness of digital pathology for mainstream clinical practice and could pave the way for the adoption of similar technologies in other areas of medicine. Unlike Scotland's approach of focusing on MRI-first pathways, this study specifically targets the biopsy analysis stage, potentially offering a complementary layer of precision.
Local Impact
For the local communities in Oxford, Bristol, and Glasgow, the study offers the immediate benefit of access to cutting-edge diagnostic technology. Men diagnosed with prostate cancer at the participating NHS trusts will be among the first in the country to have their cases reviewed using this advanced tool. This could lead to more personalised and effective treatment plans for individuals in these areas. In the longer term, if the technology is rolled out across the NHS, the impact will be felt in every community in the UK and Ireland. Every man diagnosed with prostate cancer will have the opportunity to benefit from a more precise and personalised diagnosis, leading to better health outcomes and a higher quality of life for patients and their families.
What's Next
The VANGUARD PATH study is now underway, and the research team will be working intensively over the coming months to implement and validate the technology. The results of the study will be eagerly awaited by the medical community, patient advocacy groups, and health policymakers. If the findings are positive, Prostate Cancer UK will work with the NHS to develop a strategy for the national rollout of the ArteraAI tool. This will involve addressing a range of practical issues, including regulatory approval, data governance, and the training of healthcare professionals. The study is expected to take several years to complete, but the insights it generates will be invaluable for the future of cancer care.
Sources: Prostate Cancer UK | Sky News