HSE Health and Safety Function Rated High Risk After Decade Without Approved Mandate
An internal audit of Ireland's Health Service Executive has assigned a high risk classification to the potential for serious incidents within the healthcare system, after finding that the National Health and Safety Function has been operating without an officially approved mandate since 2015 — and that 16 of 33 acute hospitals lack a dedicated, full-time health and safety officer.
Background
The HSE is the largest employer in Ireland, responsible for the delivery of health and social care services to a population of over five million people. It operates a network of acute hospitals, primary care centres, mental health services, and disability services across the country, employing over 130,000 staff. The scale and complexity of the organisation makes robust health and safety governance not merely a regulatory requirement but a fundamental operational necessity.
The National Health and Safety Function (NHSF) was established to provide strategic leadership and oversight of health and safety across the HSE. Its mandate covers everything from infection control and manual handling to the management of violence and aggression in clinical settings. The function is supposed to set standards, monitor compliance, and support frontline services in managing the risks inherent in healthcare delivery.
The HSE has faced significant scrutiny in recent years over its governance and management practices. The catastrophic ransomware attack of 2021, which brought the health service's IT systems to a standstill for weeks, exposed deep vulnerabilities in the organisation's resilience. The Slaintegare reform programme, intended to transform the health service over a decade, has faced repeated delays and implementation challenges. Against this backdrop, the findings of the internal health and safety audit are particularly concerning.
Key Developments
The internal audit, detailed by TheJournal.ie on 4 May 2026, found that the NHSF has been operating without an officially approved mandate since 2015 — a period of over a decade. This fundamental governance failure means that the function has been carrying out its work without a clear, formally sanctioned basis for its authority, creating ambiguity about its powers and responsibilities. The audit assigned a high risk classification to the potential for serious incidents to occur as a result of these shortcomings.
The audit also identified a critical staffing deficit: 16 out of 33 acute hospitals in the country lack a dedicated, full-time health and safety officer. This means that nearly half of Ireland's acute hospitals are managing health and safety risks without the specialist expertise that the role provides. The absence of dedicated officers raises serious concerns about the ability of these institutions to identify hazards, investigate incidents, and implement corrective measures in a timely and effective way.
Separately, the HSE's spending on agency workers has surged by over €100 million, which Sinn Fein's health spokesman described as a complete waste of taxpayers' money. The combination of governance failures, staffing deficits, and rising agency costs paints a troubling picture of an organisation under severe strain.
Why It Matters
Health and safety failures in hospitals are not abstract governance concerns — they have direct consequences for patients and staff. When hospitals lack dedicated health and safety officers, risks go unidentified, incidents go uninvestigated, and lessons go unlearned. The HSE's own audit has identified this as a high risk situation, which in the language of risk management means that the likelihood and potential severity of harm are both significant.
For context, the UK's NHS has faced its own health and safety challenges, but the regulatory framework — overseen by the Health and Safety Executive in Great Britain and the Health and Safety Executive for Northern Ireland — provides a more robust external check on compliance than exists in the Republic. Ireland's Health and Safety Authority has jurisdiction over the HSE, but the internal audit's findings suggest that internal governance has been inadequate for over a decade. This is the kind of systemic failure that, if left unaddressed, creates the conditions for serious incidents.
Local Impact
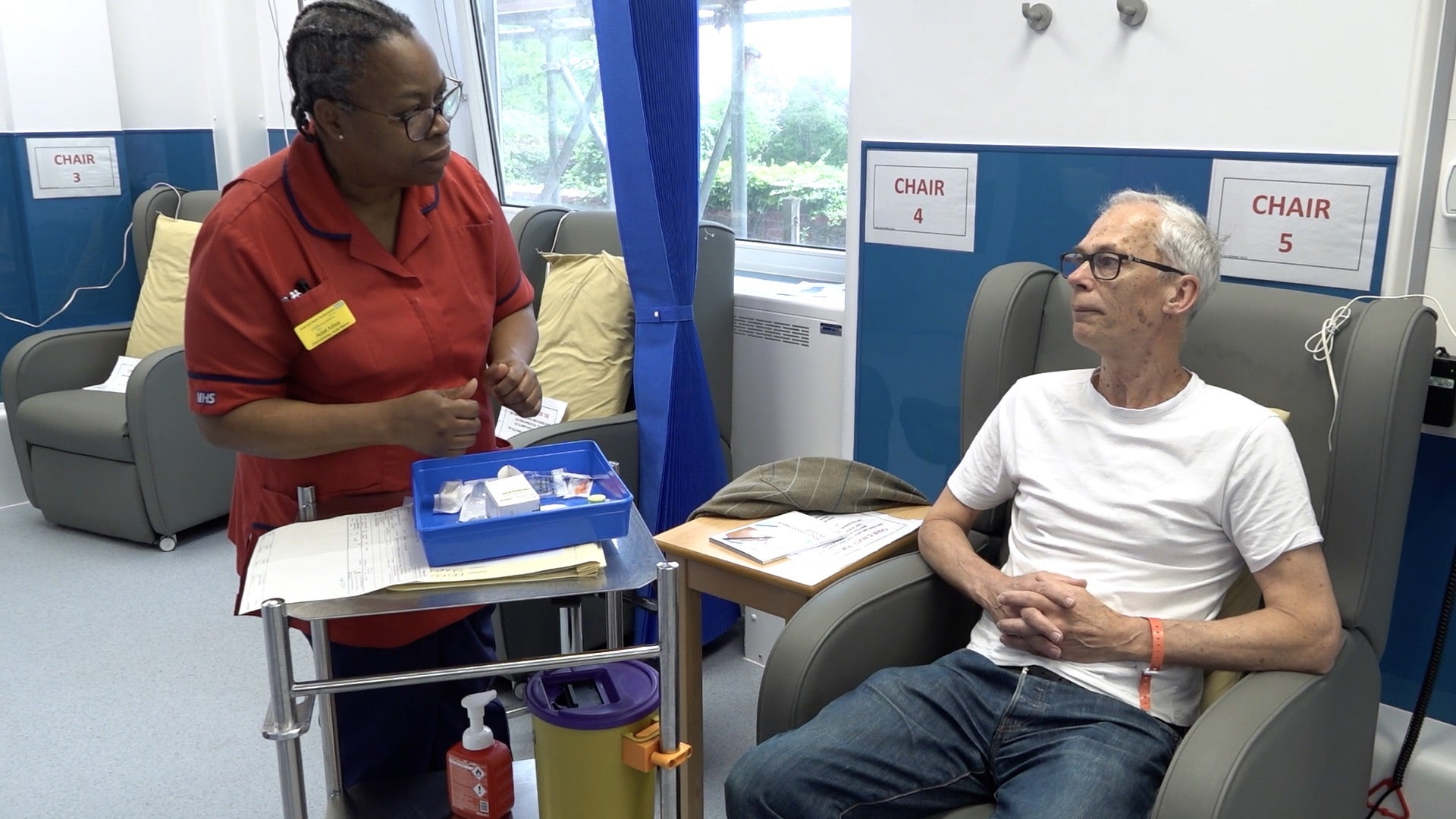
For patients and staff across Ireland's acute hospital network, the audit's findings are deeply concerning. The 16 hospitals without dedicated health and safety officers include institutions serving communities across the country, from major urban centres to rural areas where the local hospital is the only acute facility for miles around. For healthcare workers — nurses, doctors, porters, cleaners — who face daily risks including needle-stick injuries, violence from patients, and musculoskeletal strain from manual handling, the absence of specialist health and safety support is a real and immediate concern. In Northern Ireland, where the Health and Social Care system operates under a different regulatory framework, the findings will nonetheless prompt reflection about whether similar gaps exist.
What's Next
The HSE is expected to respond formally to the audit's findings, setting out a timeline for addressing the identified deficiencies. The establishment of an approved mandate for the NHSF and the recruitment of health and safety officers for the 16 hospitals currently without them are the most urgent priorities. The Health and Safety Authority is likely to seek assurances from the HSE about its plans for remediation. The Oireachtas Health Committee is expected to seek a briefing from HSE management on the audit's findings and the organisation's response.
Sources: TheJournal.ie — HSE health and safety audit; Irish Examiner — Irish health news